TMS Therapy Near Me: How to Find the Right Provider
Not all TMS providers are equal
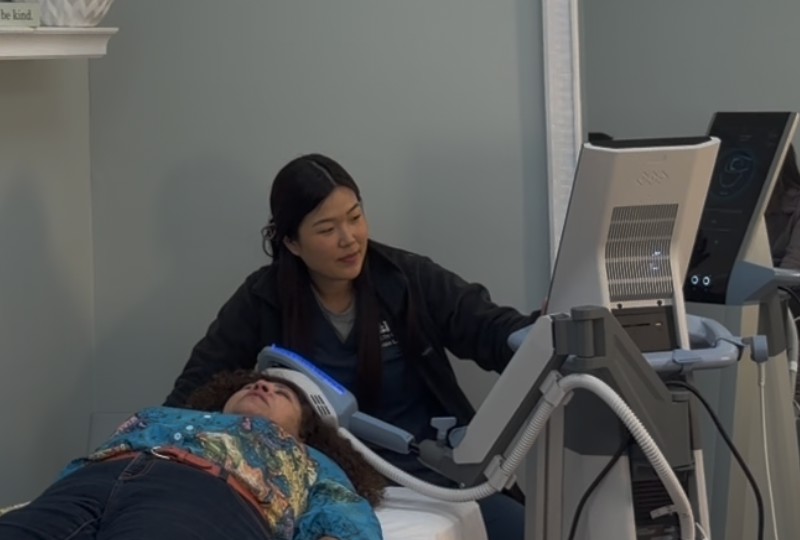
You typed "TMS therapy near me" into a search bar.
That search represents something significant. It means you've moved past the stage of wondering whether to try TMS. You're trying to figure out who to trust with your brain health.
That is exactly the right question to be asking. And I want to help you answer it honestly.
Here's what most people don't know: TMS is not a commodity. Two clinics can both offer "TMS therapy" and deliver completely different levels of care, precision, and outcomes. The equipment matters. The protocol matters. The clinical oversight matters. The physician behind the treatment matters enormously.
I've been practicing TMS in primary care for years. I've seen what excellent care produces—and I've heard from patients who experienced less than that elsewhere. So let me give you the inside view on how to evaluate a TMS provider before you commit.
What TMS Actually Is (and Why Provider Quality Matters)
Transcranial magnetic stimulation works by delivering precise magnetic pulses to specific regions of the brain—primarily the dorsolateral prefrontal cortex—to stimulate underactive neural circuits and promote neuroplasticity. When it's done correctly, with the right protocol and the right targeting, it produces outcomes that nothing else can match: 88% response rates, 72% remission rates in published real-world data.
When it's done carelessly, with generic protocols, undertrained staff, and minimal physician oversight, it can produce underwhelming results that leave patients concluding TMS "didn't work"—when what actually happened is that that particular clinic's version of TMS didn't work.
The difference between a great TMS provider and an average one is the difference between precision medicine and an assembly line. You deserve to know which one you're walking into.
7 Questions to Ask Any TMS Provider Before You Start
- Who oversees my care, and will I have access to a physician?
This is the most important question. TMS should be physician-led—not delegated entirely to technicians who run sessions while the doctor is nowhere in the building. Ask: who evaluates me for candidacy? Who designs my treatment protocol? Who do I call if I have questions or concerns during treatment?
At a high-quality practice, a physician is involved at every critical decision point. At a lower-quality practice, you may see the doctor briefly at intake and then never again.
2. What protocol do you use, and why?
There are multiple TMS protocols—traditional rTMS, intermittent theta burst stimulation (iTBS), accelerated formats, and others. Each has different evidence bases, session durations, and delivery models. A provider who can't clearly explain what protocol they use, why they use it, and how it's calibrated to your individual brain is not practicing precision medicine.
Ask specifically: Do you use iTBS or traditional rTMS? How do you determine my motor threshold? How are sessions spaced? What is the total pulse count?
3. What are your actual outcome data?
Most clinics will tell you TMS "works." Ask them to show you their numbers. What is their response rate—meaning the percentage of patients who experience significant improvement? What is their remission rate? How do they define and measure those outcomes?
Be specific: ask for PHQ-9 and GAD-7 data, not just testimonials. Testimonials are moving. Data is evidence.
If a clinic can't show you their outcomes, that's a meaningful piece of information.
4. How is my treatment personalized?
Off-the-shelf TMS protocols treat every brain the same. Individual motor threshold testing—measuring the precise stimulation intensity needed to activate your specific neural circuits—is a minimum standard. Beyond that, ask whether the clinic evaluates your broader health picture: thyroid function, hormonal status, sleep quality, inflammatory markers. These factors directly affect treatment response.
A physician who integrates primary care with TMS will find things a siloed psychiatric evaluation misses. That matters for outcomes.
5. What happens after the treatment?
TMS is not a one-and-done intervention. Follow-up, maintenance protocols, and access to booster sessions when needed are part of comprehensive care. Ask: how do you monitor my progress after the initial course? What's the plan if symptoms begin to return? Do you offer ongoing care or does the relationship end after my last session?
6. What is your safety protocol, and what are the contraindications you screen for?
A credible TMS provider will screen carefully for contraindications: metal implants near the head or neck, history of seizures, certain cardiac devices. They will have a clear protocol for adverse events and will educate you on what to expect before, during, and after treatment.
If a provider rushes through contraindication screening or doesn't clearly explain the safety profile of TMS, pay attention.
7. Have you treated patients like me?
This sounds simple, but it matters. Treatment-resistant depression is not the same as mild depressive episodes. Anxious depression is not the same as pure anxiety disorder. PTSD presents different neurological patterns than GAD. Ask whether the provider has experience with your specific presentation—and ask what outcomes they've seen.
Red Flags That Should Send You Elsewhere
They can't tell you their outcomes data. Every credible TMS practice should track and be able to share patient outcomes. If they deflect to "we've seen great results" without specifics, that's a red flag.
Minimal physician involvement. If you're told you'll see the doctor once at the start and that's it, think carefully. TMS is medical treatment. It requires medical oversight.
Generic protocols with no individualization. If the clinic doesn't discuss motor threshold testing, personalized protocol design, or your broader health picture, you're being processed, not treated.
High-pressure sales tactics. A legitimate TMS provider wants to determine whether TMS is the right fit for you—not close a sale. Be wary of urgency tactics, package deals that pressure quick decisions, or clinics that don't ask enough questions about your history before recommending treatment.
No discussion of contraindications. If the intake process doesn't involve a careful review of contraindications, the clinic is either careless or understaffed for proper clinical oversight.
Technician-only operation. TMS equipment can be operated by trained technicians, but the clinical judgment that determines protocol, dosing, and appropriateness of care requires physician expertise. Make sure you know who is making those decisions.
Should You Travel for Better TMS Care?
This is a question I get often, and my answer is always the same: it depends on how important this outcome is to you.
If you've tried multiple medications without adequate relief, if you've been labeled treatment-resistant, if you are genuinely suffering—then a 2-hour flight for care that has an 88% response rate is a very different calculation than a 30-minute drive for a clinic with unknown outcomes.
The KIND One-Day Protocol was specifically designed with this in mind. By compressing a full TMS course into a single day, we made it possible for patients to travel from across the country—and the world—to access physician-led, precision TMS without needing to relocate or clear their schedules for six weeks.
We have patients who fly in from New York, Chicago, Texas, and beyond. They come for one day. They leave with a completed treatment course. And they follow up remotely while results develop over the following weeks.
If you have access to a high-quality TMS provider in your area, wonderful. If you don't—if the options near you feel generic, technician-driven, or outcome-opaque—it is worth asking whether traveling for better care makes sense.
Your brain health is worth that conversation.
What to Look For in a High-Quality TMS Practice: A Quick Checklist
Use this as your evaluation guide:
✅ Physician-led, with active physician involvement throughout your care
✅ Clear, specific protocol (iTBS or well-justified traditional rTMS)
✅ Individual motor threshold testing for precision dosing
✅ Published or demonstrable outcomes data (response and remission rates)
✅ Integration with comprehensive health evaluation (not just psychiatric history)
✅ Clear plan for follow-up, maintenance, and access to boosters
✅ Thorough contraindication screening
✅ Transparent pricing and no high-pressure sales tactics
✅ Experience treating your specific presentation (depression, anxiety, PTSD, etc.)
✅ You feel genuinely heard and evaluated, not processed
What Makes Kind Minds Different
I want to be transparent about who we are and what we offer—not to pitch you, but because you deserve to know what physician-led, outcomes-driven TMS actually looks like in practice.
Kind Minds was founded on a simple premise: patients with treatment-resistant depression deserve access to the most effective, most precise, most clinically rigorous TMS available. Not convenient TMS. Not franchise TMS. The kind of care that produces results.
Everything we do is built around that commitment:
- Every patient is evaluated by me personally. Dr. Georgine Nanos, MD, MPH—a board-certified family physician with over twenty years of clinical experience.
- Every protocol is individually calibrated to the patient's motor threshold, health history, and specific presentation.
- Our outcomes are published. 88% response rate. 72% remission rate. Among the strongest real-world TMS results ever documented.
- We integrate primary care with TMS. We look at the whole system—not just the psychiatric symptom. We find root causes that other evaluations miss.
- The KIND One-Day Protocol means one visit, one day, full therapeutic course. We built this specifically for patients who can't commit to a six-week schedule—and it works.
If you're evaluating TMS providers and you'd like to understand whether Kind Minds is the right fit for you, I'd welcome that conversation. Not to sell you anything. Because you deserve real information to make an informed decision.
Ready to Talk?
Our complimentary consultation is exactly what it says: a real clinical conversation. We'll review your history, discuss your goals, assess your candidacy, and give you honest answers about what TMS can and can't offer you.
No pressure. No scripts. Just information.
Schedule Your Complimentary Consultation
Disclaimer: This content is for informational purposes only and does not constitute medical advice. TMS may not be appropriate for everyone. Please consult with a qualified healthcare provider to evaluate the right treatment for your individual situation.
About Kind Minds
Kind Minds, founded by Dr. Georgine Nanos, MD, MPH, is a physician-led TMS practice in Encinitas, California. We specialize in treatment-resistant depression, anxiety, PTSD, and related conditions through the KIND One-Day TMS Protocol. Our published research documents response rates of 88% and remission rates of 72%—among the strongest outcomes ever reported in real-world TMS practice.

Meet the Author
Dr. Georgine Nanos, MD, MPH
Founder of Kind Health Group